NEW DELHI — When India began reeling from a disastrous second wave of Covid-19 in June, Aparna Kumar parked her car in front of a private hospital in the capital’s affluent South Delhi district, and opened her phone to log onto CoWin, the Indian government’s website for vaccine registrations. The 43-year-old homemaker, who has long black hair and a jovial disposition, had stepped out of her home for the first time since March, when the virus began to spread among her friends and neighbors. In the months that followed, cases were rampant in her entire neighborhood; an elderly man next door died. By some miracle, Kumar and her family remained healthy. Not wanting to take any risks, she ordered everyone to stay in and sealed off even their balcony in case the virus was spreading in the air outside. “We live wall-to-wall with people,” she told me. “If one person gets sick, everyone in the family gets sick.”
But when Kumar was finally eligible for the vaccine in May, she hesitated to get her shot. “I’d heard so many different things, I was worried,” she said. Even when her in-laws, husband and son all got their first doses, she held back from booking an appointment. Misinformation floating around on WhatsApp convinced Kumar, a diabetic, that the vaccine would make her condition worse. But pressure to get the vaccine began mounting from her family. Now, as she stood in front of the hospital, which had converted an entire floor into a vaccination center, she contemplated the shot with trepidation. “I’ve basically been dragged here,” she told me at the time, laughing nervously.
Vaccine hesitancy is one of the many reasons women are being left behind in India’s inoculation drive, which has so far fully vaccinated less than 4 percent of its adult population since it began in January. Government data reveals nearly 17 percent more men than women have received a shot. Of the 729 districts for which data is available, more men have been vaccinated in as many as 620 districts. Across 16 states and union territories, including some of the most populated like Uttar Pradesh, Bihar and even Delhi, women have not outnumbered men.
“Women have taken a back seat while men are getting vaccinated,” said Aditi Madan, a doctor and associate fellow at the Institute for Human Development, a non-profit research organization in Delhi.
In interviews, a dozen women across India expressed doubt over the vaccine. Like Kumar, nearly all had heard rumors and misinformation about the vaccine’s effectiveness. Vaccine hesitancy has been a big factor among the general population in allowing the virus to spread unabated, but not only the reason women are getting left behind. Those who want to get vaccinated also face a lack of access: urban women have spent days trying to find slots on CoWin due to glitches in the registration system and a vaccine supply shortage, while women from lower-income and rural communities are rarely prioritized, don’t have smartphones or mobile data, and can’t afford to take time off from work to travel to a vaccination center.
India’s gender bias has prohibited women from accessing health care more generally: A 2019 study conducted by experts from India and Harvard University revealed that factors like age and geographical location determined if they could get to a hospital, while gender stereotypes prevented them from voicing their health problems. The health care system has made some strides over the last few decades, with women attaining a higher life expectancy and a lower maternal mortality rate. But the accessibility and affordability of health care services also affected women’s growth and development; non-communicable diseases like diabetes and hypertension have risen, replacing traditional causes of death. In 2014, the Health and Family Welfare Ministry launched an ambitious immunization program called Mission Indradhanush, the world’s largest . Its aim was to try to fill the gaps by protecting women and children from diseases like tuberculosis and polio. But coverage has varied considerably, with women and girls receiving fewer vaccinations than men and boys, according to Unicef.
Closing the gender gap in India’s COVID-19 vaccine rollout hasn’t received the kind of attention it should have, Madan said, particularly because the government has been busy responding to other criticism. “Because [women] stay at home, it’s easy to think why spend the extra time and money?” she said.
“But it’s an issue that’s here to stay,” she added. “The implications it can have on the whole family are huge.”
In many developing countries, women face limited mobility to reach vaccination sites, restricted decision-making power over matters of their health, and limited access to information about vaccines and vaccine safety, according to the World Health Organization (WHO). “When women have access to health services and can lead healthy lives, the whole country benefits,” said Karina Gould, Canada’s minister of international development, at a recent WHO event addressing gender equality in the Covid-19 vaccine roll out. “By now, we all know that no one is safe until all of us are safe.”
But in India, ensuring women’s access to healthcare has also been exacerbated by a glaring divide between the rich and the poor. Since launching India’s inoculation drive—in January, for frontline workers and anyone over 60; in April, for anyone over 45; and in May, for all adults over 18—the government has come under fire for its botched rollout, an oversight that has contributed to the 29 million cases and 180,000 deaths that accumulated during the second wave and resulted in the world’s second-largest Covid-19 outbreak. Those are the official numbers, the real death toll is widely considered to be much higher.
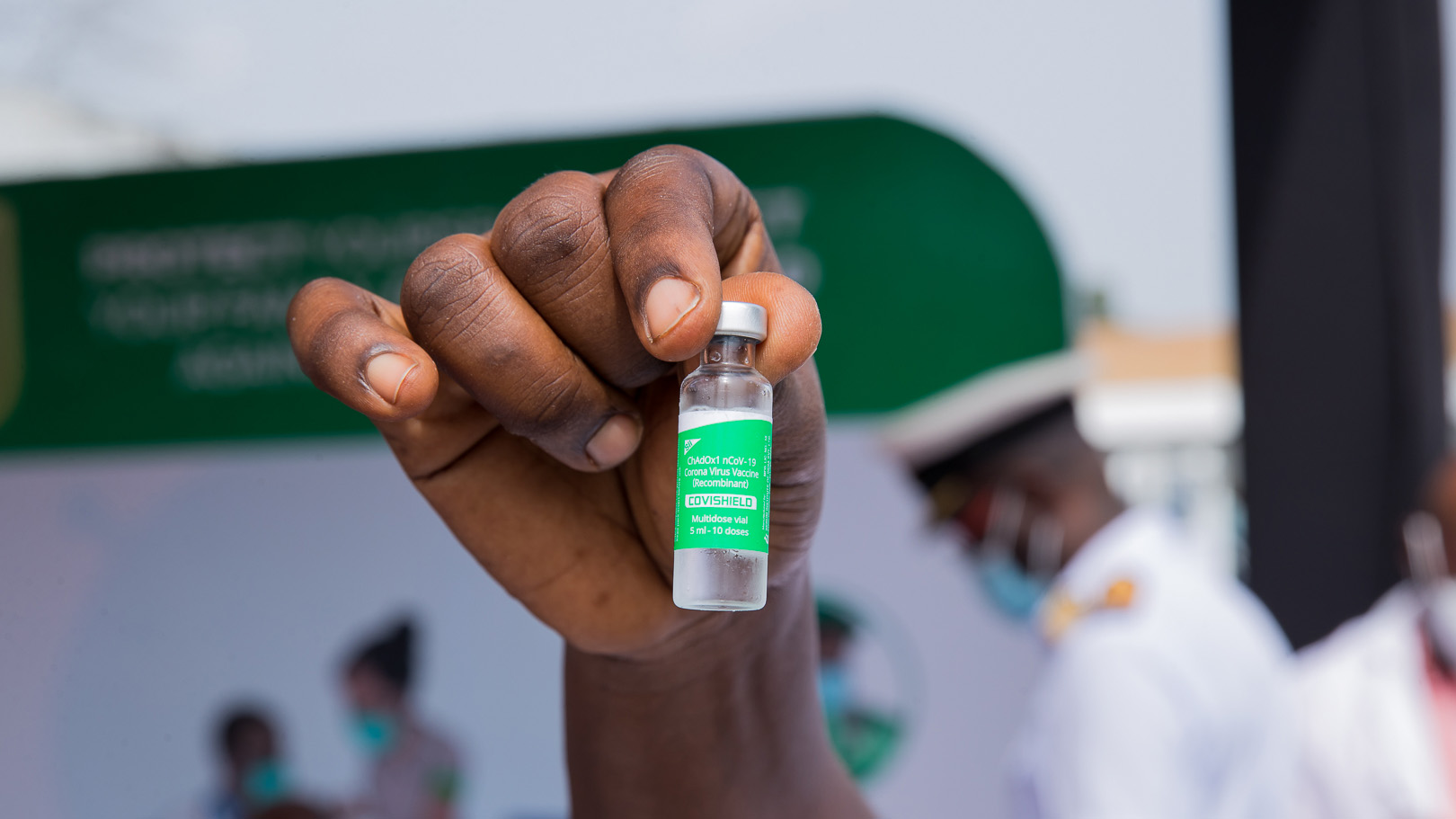
At the beginning of the year, many Indians had high hopes for a vaccine, considering their country had established itself as the world’s largest vaccine maker. The domestic production of two Covid-19 vaccines was underway: Covishield, the Indian version of the AstraZeneca vaccine made by the Serum Institute, and Covaxin, a locally developed vaccine made by the Indian company Bharat Biotech. But India only placed its first orders for 11 million doses in January, while simultaneously donating more than 66 million doses to 90 other countries.
High hopes for vaccines were matched by equal levels of complacency and overconfidence. The health minister declared that India was in the “endgame” of the pandemic in March, and a sense of normalcy took over. Mass public gatherings began taking place again, enabling the virus to spread again—this time through new variants at a much faster rate. As cases surged by April, the clamor for vaccines also increased. Prime Minister Narendra Modi accelerated the timeline of the vaccination program by months, allowing all adults to get vaccinated from May 1 despite a severe shortage of vaccines. Then his government passed the buck, requiring states to acquire their own doses, leaving them scrambling to place orders from manufacturers.
Only 600,000 people, or 1.3 percent of the eligible population, registered on CoWin initially, many belonging to India’s privileged classes. Even for them, finding an open slot in the system is like winning the lottery: people sign onto CoWin at odd hours of the night, or rely on hacks using bots and applications to find slots. But with half the country with no access to the internet, those in smaller towns and rural areas have little to no hope of getting any slot. In an attempt to get around its vaccine shortage, the government has doubled the gap between the two doses of the AstraZeneca vaccine, which accounts for nearly 90 percent of the 257.5 million vaccine doses administered so far, from 6-8 weeks to 12-16 weeks. The decision came without the agreement of the scientific group the government claims recommended this increase, according to a Reuters report.
But supply shortage isn’t the only issue facing India: reports about rushed production, the lack of clinical trials and efficacy data have also surfaced. Misinformation circulates at a rapid rate, too, with many Indians convinced by rumors that the vaccines contained pig meat and cow blood, sparking religious concerns among Hindus and Muslims, and that they could cause infertility and death.
The inequity underlying India’s immunization drive has meant that the country has given one dose to a much lower proportion of its 1.35 billion citizens than other countries like the United States, Brazil and the United Kingdom. To appease critics, Modi’s government made vaccines free for all adults from June 21 under the federal government’s program.
* * *
When the second wave of the pandemic hit, Kajal Kohinoor, who works as a domestic maid for many affluent homes in Delhi, realized her mother had fallen ill with all the obvious symptoms of Covid-19. In their one-bedroom slum dwelling in an urban squalor in Dwarka, an area on Delhi’s southwestern fringe, the 27-year-old and her husband, a taxi driver, hoped to nurse her mother to full recovery. But when her condition deteriorated, Kohinoor had no choice but to ask her employers for help: she needed medicine, and wanted to take leave so her family could return to her village in Samastipur in the eastern state of Bihar. “I told madam the water in the village will be good for my mother,” she said.
Kohinoor has been living in the village with her in-laws since April. At first, she was scared of the vaccine when she saw people dying in her village, especially those who had taken their first doses. But her employers urged her to get the shot: “Madam keeps saying [the vaccine] will be good for me and that my kids will be safe,” she said. Last week, her in-laws finally got vaccinated at a local clinic set up by the government, 10 minutes away from her village. These assurances boosted her confidence to get the jab, but when she asked the local anganwadi worker, or social worker, to administer it at the clinic, she was told only people over the ages of 45 were eligible in the area. “They told us they don’t have any stock for us yet,” she said. When the village will get more vaccine supplies for all adults is anyone’s guess. And without their monthly wages, Kohinoor and her husband are starting to feel the pressure to return to Delhi soon. “Maybe we can finally get the vaccine there,” she said.
Over 65 percent of India’s population resides in rural areas, according to World Bank data, leaving a widespread gap between wealthy and poor Indians, that leaves large swathes of the country’s population vulnerable to Covid-19. In May, Boston Consulting Group’s Covid-19 Consumer Sentiment Survey found that 63 percent of Indians in rural areas and 43 percent in smaller towns didn’t know how to enroll in CoWin, with a smaller percentage not knowing they had to enroll at all. Those who hadn’t received the vaccine despite it being available said they faced issues with registration and lack of slots. A BBC analysis found that among 729 districts for which data was available, some districts had given jabs to half their populations, while others had vaccinated as little as 3 percent. Recently, the Supreme Court took the federal government to task over the disparity: “How will an illiterate laborer from Jharkhand get registered in Rajasthan?” one of the judges asked the solicitor general Tushar Mehta. “Tell us how you will address this digital divide.”
Madan, of the Institute for Human Development, has some ideas. Public health centers in rural areas can be converted into vaccination centers, she said, and community health workers (also known as ASHA workers), who have historically played a big role in immunization drives, can help persuade more women to come forward for their shots. “Women are instrumental in their roles as caregivers and in carrying out public health work,” she said.
The burden of caring for the sick and meeting the family’s needs commonly falls on women during disasters, notes Susan Ferguson, the UN women representative for India. In both the first and second pandemic wave, women have provided the bulk of health care in both clinical settings and at home. Their exposure to the coronavirus has remained high, while their own health care needs have been poorly addressed. But the inclusion of women is key to strengthening health systems, a report by the George Institute for Global Health in India states. “A woman empowered with knowledge about the disease and risk factor burden can be transformative to the health of entire families.”
It seems unlikely Kohinoor will get vaccinated soon even when she returns to Delhi. Her friend Sanju, who lives in the same neighborhood of Dwarka, said no one there has had the vaccine so far. “We’re all waiting,” the 28-year-old said. Like Kohinoor, Sanju also works as a domestic maid, cleaning three different houses every day. All the members of every household she cleans have been vaccinated. “They told me, ‘We can’t get you vaccinated because we went to a private clinic,’” she said. Sanju would rather wait for a free dose than pay for one. She and her husband, a daily wage laborer, have to support their two kids, aged 10 and 11. “We don’t have that kind of money, we couldn’t even eat during the lockdown,” she said. She doesn’t own a phone and uses her husband’s sparingly, relying on hearsay for vaccine updates.
Recently, she heard the local council might set up a free vaccination camp at a nearby school once the state government receives more doses. While some villagers are skeptical, she has no qualms about getting the jab. “If all these educated people are doing it, why should I hesitate?” she said. But until then she is remaining alert, wearing a face mask and paying attention to anyone around her showing signs of sickness. “My kids are small, so I can’t afford to get corona,” she said.
* * *
I received my first dose of Covishield in May at the same hospital in South Delhi where I met Kumar. Terrified by the vast number of cases and deaths overwhelming the city’s hospitals and crematoriums, I made a desperate call to a doctor at a private clinic and was immediately able to book a slot for later in the week. I was relieved at the ease of the process, but also bewildered given the desperation of countless others trying to book their own slots. The vaccination center was a mile from my apartment and I turned up armed with gloves, double masks and a durable face shield, paying a total of 250 rupees ($3.44) to get my shot. There was no escaping it: I had benefited from my privilege in the most obvious way.
As I stood by the vaccination center talking to women about their experiences getting the jab a month later, most also reflected this privilege. Shimla Singh, a 31-year-old project manager at a market research company, said her process to book an appointment was “effortless.” She said she has had many doubts over the vaccine’s safety: “There are still a lot of questions on my mind, so it still isn’t set.” In May, she had read a few theories being peddled on WhatsApp suggesting the vaccine could lead to excessive bleeding and acute pain during menstruation, impacting women’s fertility. The theory gained widespread traction, leading to anxious calls to a helpline run by the Department of Women and Child Development. Madan believes that policymakers have a big role to play in carrying out awareness campaigns to help clear misconceptions. “It becomes really important to become women’s advocates and persuade more women to come forward for their jabs,” she said.
Singh’s office recently made getting at least one dose of the vaccine mandatory for returning to the office, so she spent nearly two weeks trying to book her slot before she finally got vaccinated, more because of necessity than choice. She hopes to return to her office at the end of June.
But Kumar felt a huge wave of relief after she got her shot. Handing the nurse her phone, she even asked for a picture in front of the hospital’s designated vaccine photo-booth. In her white and gold lace salwar-kameez, she posed with a smile on her face, holding her arm up. “So my whole family knows I finally did it!” she exclaimed. “It was so quick!” she said, reemerging onto the street. She told me she paid 780 rupees ($10.53) for her Covishield shot—almost triple the price I had paid just months earlier, reflecting an arbitrary system dictated by private hospitals. For Kumar, however, the price paled in comparison to the relief she felt. “I’ve tried everything I could find to keep myself safe since last year. Steaming, homeopathic medicines, Vitamin C, you name it,” she said. “But the fear I had, I feel like it’s finally passing.”
When Kumar left, Shromani Ramkishen Divakar, who works as an entrance guard at the vaccination center, came up to me with a colleague. The pair had been observing my conversations. Divakar was a short, sturdy 38-year-old woman dressed in coral uniform, from a village in the Etawah district in Uttar Pradesh. She had received a free dose as a frontline worker back in March, but said her family members in the village were still waiting. Referring to Kumar, she said pensively, “Her whole family paid at least 3,000 rupees to get the vaccine. Almost half our salary.”
“If the government can give free vaccines to doctors and workers, why do the rest of us have to wait so long?” she asked. Although vaccines are now free for all Indians and the government has mandated that registering on CoWin is no longer compulsory, their availability still depends on how well-equipped states and districts are with vaccine supply.
Divakar’s colleague, a 46-year-old man named Jayashankar Prasad, chimed in. He told me he had seen the most horrific scenes in April and May while working at the hospital: body after body arriving day and night, gasping for breath. “I’ve learned one thing: We need to save ourselves, the government will not come to save us,” he said.
I asked Prasad if he and his family had gotten their shots. “I got mine last month,” he said. “But my wife, what’s the need? She stays inside the house,” he shrugged.
“I’ll get her vaccinated eventually.”
Top photo credit: UK Department for International Development, Wikimedia Commons




