NEW DELHI — When public hospitals across India began preparing for an onslaught of Covid-19 patients in March, Merin Thomas, a nurse at the city’s All India Institute of Medical Sciences (AIIMS), volunteered for the newly formed Covid Intensive Care Unit. Some 80 medical workers had signed up; Thomas was in the first of three groups to work long 14-day shifts.
While some of her colleagues had volunteered to go to the front line instinctively, the decision did not come easily for Thomas. She lives at home with her parents, both in high-risk groups, one with diabetes and the other hypertension. Her mother is also a nurse in a public hospital.
“Since I work in a hospital, I understand that I’m always surrounded by infections,” she said. “But when I come back home, I’m worried about infecting them.”
The 26-year-old is one of over 12 million essential workers—dubbed “Covid warriors”—currently on the front lines preventing the spread of the virus, which by the end of April had reached some 33,050 people across the country, killing 1,079 people, according to the Health and Family Welfare Ministry.
In a population of over 1.3 billion, only 0.004 percent has been infected so far. Compared to Canada, which has had almost as many cases, the fatality rate is much lower, with half as many reported deaths. And while counting mortality rates in India has always been an inexact science—only 22 percent of deaths are medically certified—there also have been no reports of a massive surge in Covid-related hospital deaths yet.
Doctors, nurses and paramedics face not only higher risk of exposure but also a constant fear of attacks from the social stigma that now overshadows the pandemic. Notably, it is women—who constitute almost half the country’s health workforce and 90 percent of its nursing staff—who tend to shoulder the burden more in both formal healthcare settings and at home.
The coronavirus has infected around 548 doctors, nurses and paramedics so far in central and state government-run facilities, according to a report by the Press Trust of India. The stressful and at times dangerous working conditions under Covid have led many medical associations to demand better laws for protection and intervention by the government. However, with the easing of lockdown restrictions looming, it remains to be seen whether healthcare workers will be able to cope with country’s rising number of infections.
The toll on medical workers
As a psychiatric nurse working in critical care who is familiar with the sight of ventilators and emergency equipment, Thomas assumed she was well-prepared to work in the Covid ICU.
But in the days leading up to her posting, she became anxious. She had read news reports about many people dying from the virus and healthcare workers under attack. “I started doubting myself and wondering, ‘Will I be able to handle this?’” she said.
In training sessions, doctors and nurses were given detailed practical instructions on how to don and doff personal protective equipment (PPE) during rotating shifts. While AIIMS is a prestigious government hospital with no shortage of PPE, many other hospitals have repeatedly faced a scarcity of masks and testing kits, according to several media reports. To meet the demand, India began producing its own PPE rather than relying on imports. In the two months since the outbreak, it has gone from producing no PPE kits to over 150,000 kits daily.
Inside the unit, a group of nurses work with patients while another assists with equipment and maintenance of patient records outside. They are instructed to eat, drink and use the restroom right before they start their shifts; once inside with Covid patients, they are not able to leave.
On her first shift, Thomas was sent inside a Covid ward to work alone, assisting a single doctor and a health associate with the treatment of five patients. A four-hour shift usually went by quickly, but on that day, Thomas felt desperate to pull off her mask by the third hour. “There was a lot of air hunger and I was suffocating inside,” she said.
In a screening area in the hospital’s emergency department, nurses examined the patients’ medical and travel histories, and checked for symptoms. Those who exhibited the “three cardinal symptoms” of coronavirus—fever, cough and breathing difficulties—were sent to a separate Covid ICU. In this zone, Thomas would again check for symptoms, take nasal and oral samples, and send tests to the virology unit. The results usually came back in under six hours; patients who tested positive were moved to a ward with other Covid-positive patients in another building.
In the fourteen days she worked inside the ICU, Thomas witnessed five deaths: “We don’t usually get that many, and a lot of those patients were intubated.”
But her most grueling experience by far was caring for an 11-month-old baby left alone in the Covid unit for 12 to 18 hours. “He was crying a lot,” Thomas recalled. “He couldn’t be fed so I had to give him nutrition through an IV drip. Eventually, I had to sedate him to help him sleep.”
“Can you imagine a baby, without his parents, with people who looked like aliens dressed in hazmat suits from head to toe?” she recalled.
A shortage of separate accommodations for healthcare workers, along with the need to prioritize older staff with children, meant Thomas would have to return home after every shift and maintain social distancing. “I was living in the same house but staying inside my room, and that hurt,” she said. “I couldn’t sit with my parents for meals or chat with them like I normally would, or even give them a hug.”
By contrast, two of her male colleagues relocated their families back to their hometowns prior to starting their shifts, a kind of flexibility Thomas could not enjoy. In India, women must often balance work responsibilities with domestic chores like cooking and cleaning, particularly for male family members.
“[My colleagues] were bachelors again, but where are [women] supposed to send our families, who are dependent on us?” Thomas said.
To make things worse, three weeks after completing her shifts and resuming normal duties at the hospital, Thomas received an alarming message from her mother: “Merin, I’ve been admitted [to the hospital].”
After a doctor at her mother’s hospital had tested positive, she was placed under quarantine at the hospital. Thomas and her father did not see her mother for three days; they communicated only through video calls.
Women balance work responsibilities with domestic chores like cooking and cleaning, particularly for male family members. That can leave them feeling sandwiched between personal and professional responsibilities.
Thomas’s experience is not uncommon. An analysis by Think Global Health, an initiative by the Council for Foreign Relations, cited the example of nurses in Hong Kong during the SARS outbreak in 2003, who reported “immense personal costs and feeling ‘sandwiched’ between personal and professional responsibilities.”
“Equity issues are only meaningfully integrated into emergency responses when women and marginalized groups are able to participate in decision-making,” the report noted.
Doctors ensure widespread testing efforts
Madhura Kulkarni has been practicing as a gynecologist for 27 years at her own Ayurvedic clinic in Thane, a municipality in the western state of Maharashtra. She was recently posted as a volunteer at a small, makeshift clinic in the Kajuwadi district, a residential area mixed with slums that has since become a hotspot for both Covid patients and doctors.
Kulkarni started there after responding to her local medical association’s request for private practitioners at government outpatient clinics (OPDs) to make up for a shortage of doctors. On any given day, she sees 30 to 40 patients at a time, including those with illnesses unrelated to the virus. She also makes door-to-door visits to identify potentially infected patients.
Although her current patients are vastly different from her usual elite clients—lower caste, poor and uneducated—Kulkarni has found her experience to be far more rewarding, she said. Her chief medical officer has worked in the area for 17 years. As a result, “they trust her completely, and it has made my connection with them very strong,” she said. “They are even concerned about us!”
Still, Kulkarni can see the effects that the stigma of Covid has left on them. “Nowadays, we’re not able to examine patients the way we used to,” she said. “In India especially, human touch was very common as patients wanted that reassurance. But now, we need to diagnose with limited contact, and we need to give much more consoling.”
In the same municipality of Thane just a few kilometers away, a laboratory has been conducting testing for hundreds of potential Covid-positive patients.
Back in January, a doctor named Sonal Bangde began gearing up by ordering a few test kits from Germany. “Although this particular strain is new, India has had many other types of coronaviruses before,” she said. “After Wuhan we were expecting something to come here sooner or later, especially with travelers.”
Bangde is the medical director of InfeXn, a private laboratory she founded in 2005 to conduct specialized research on infectious diseases like H1N1 and tuberculosis. Despite having trained staff to handle volatile situations, Covid-19 presents a big challenge because it requires a higher level of biosafety in addition to the high volume of cases, she said.
Acquiring test kits was difficult at first. “Many countries had stopped exporting,” she said. The supply of testing kits from Korean or US based companies is now available, but Bangde said she prefers Indian kits because their predictability rate is higher.
Rather than asking patients to come to the lab, a team of doctors is dispatched from 6 a.m. until midnight every day to patients’ homes to take samples and bring them back to the lab for testing.
Since the pandemic, the volume of calls to Bangde have shot up exponentially. She often provides reassurance to confused and anxious patients as well as testing. “When people need to get tested, there’s a lot of pain, and a lot of the questions come up about the social stigma,” she said.
That stigma has extended to her staff: one of her clinicians was told to vacate his home by his landlord, while others have had difficulty commuting due to a lack of public transportation, road blocks and extra security.

Attacks against healthcare workers rise
The stigma is far more dangerous for healthcare workers, complicating the response to the pandemic. An overwhelming 75 percent of doctors in the country have faced some kind of violence at work, according to the Indian Medical Association (IMA), a national voluntary organization representing healthcare workers.
Although that isn’t a new phenomenon in India, the extreme circumstances of the lockdown have made the general atmosphere especially hostile, according to Sanjibani Panigrahi, a psychiatrist at the New Civil government hospital in the city of Surat, in the western state of Gujarat. “It’s very discouraging, especially since you work so hard to become a doctor,” she said.
Panigrahi has been commuting to work daily since the national lockdown. One evening in early April, an angry neighbor in her building blocked her way at the entrance of her residential building when she returned home.
“I told him I’m not even in direct contact with Covid patients. I just give referrals through videos,” she said. “But he kept saying, ‘We won’t let you in, you work in a hospital and keep going in and out, you will probably get corona.’”
Panigrahi pulled out her phone to record the incident and posted the video on Twitter to draw the attention of a local member of the Legislative Assembly in Surat. To her surprise, the video went viral, the matter referred to the police commissioner as the media began to cover the incident.
Although Panigrahi’s neighbor was eventually arrested, she didn’t file an official report. “We’re not friendly obviously, but things are okay now,” she said.
Such violence persists because of a widespread suspicion among Indians that doctors commit “wrongdoing for financial gain,” according to a report by Kanjaksha Ghosh for the National Center for Biotechnology Information (NCBI).
The Indian government’s dismal spending on healthcare provides part of the explanation, going toward just 20 percent of the country’s healthcare, with the rest delivered by the private sector. With just one in nine doctors working in the public sector, effective communication between doctor and patient for the vast majority of poor Indians who can’t afford private care is seldom given importance, leaving doctors exhausted from long working hours and families angry and anxious over poor treatment.
The lockdown has exacerbated those conditions, prompting more attacks on healthcare workers around the country. Doctors have endured verbal and physical assaults, stone pelting, spitting and being chased out of patients’ homes. In others, female nurses witnessed vulgar language and obscene behavior inside hospital wards. Like Bangde’s clinician, doctors have also been evicted from their homes, while others like Panigrahi have been ostracized by neighbors because of their exposure to Covid patients. In one drastic incident in Chennai, a mob prevented the burial of a neurosurgeon who succumbed to the virus because of fear it would spread the disease in the neighborhood.
In the wake of such attacks, many medical associations have begun demanding protection for medical workers. The Resident Doctors’ Association of AIIMS wrote a letter to the Home Affairs Ministry seeking help against the forced eviction of doctors across the country. The Federation of Resident Doctors’ Association released a statement asking for better security and accountability for attacks at Covid-19 designated hospitals. In late April, the Indian Medical Association (IMA), a national voluntary organization representing healthcare workers, began to plan silent protests nationwide.
Home Minister Amit Shah responded by promising swift action, appealing to the IMA to stop the protests. Prime Minister Narendra Modi’s cabinet also issued an executive order updating the 1897 Epidemic Diseases Act “to protect each and every healthcare worker who is bravely battling Covid-19 on the frontline… There can be no compromise on their safety!” Modi tweeted.
The new laws consider violent acts against doctors to be non-bailable offences punishable by up to seven years in prison. They also provide new protections for all healthcare professions, including community local Accredited Social Health Activists (ASHA workers), consultants and lab clinicians. The government has promised compensation for injury or loss of property, along with investigations into any attacks within 30 days.
Although the measures have boosted morale, the government must ensure they are properly implemented, particularly as a new, more flexible phase of the lockdown will be introduced after May 17.
And while the workload for medics will almost certainly increase as a result of more open public spaces, for most female healthcare workers on the front lines, “thinking about the risk of taking care of our families is a major part of our lives now,” said Prerna Tayal, a resident doctor at Lady Hardinge Medical College in Delhi.
Despite the risks, she feels a renewed sense of civic duty: “I never thought that I would be part of such a big pandemic, and that I would serve my nation like this,” she said.
As for nurse Merin Thomas, she said of her time working as a nurse in the Covid ICU that talking to friends in the medical profession experiencing similar conditions was the most helpful. “They could understand my experience because they were going through the same situation,” she said. “It made me realize I wasn’t alone and I didn’t need to be a hero.”
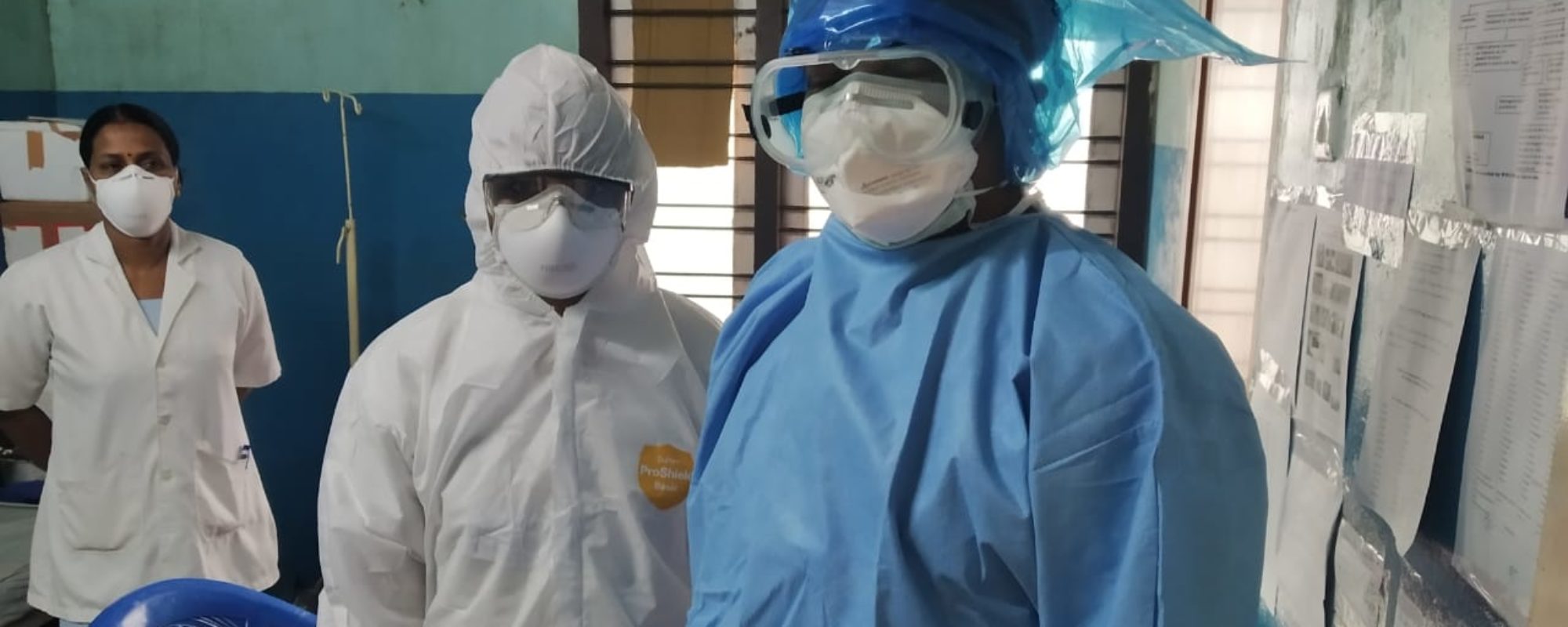
Top photo: Healthcare workers in a district hospital in Tirur, Kerala state (Javed Anees, https://commons.wikimedia.org/wiki/File:Healthcare_workers_wearing_PPE_03.jpg)